-
Procedures
Portacath
What is a portacath?
A portacath is a type of central venous line. It consists of two parts, a tunnelled line and an injection port; these are connected together underneath the skin. The tunnelled central venous line is a long, thin, hollow tube. One end of the tube (the distal end) sits just near the entrance to the heart. The other end connects to an implantable port that sits just under the skin on your upper chest. The port is usually about the size of a pound coin and is about 1 cm thick. You can usually feel the port as a small lump underneath the skin and occasionally you can see a bulge underneath the skin, especially if you are thin.
The position of the port will vary from person to person, but I will try to ensure that it is in a comfortable position and is as discreet as possible.
Many of the portacaths are ‘power ports’ which mean that they can be used for injecting intravenous contrast during CT scans.
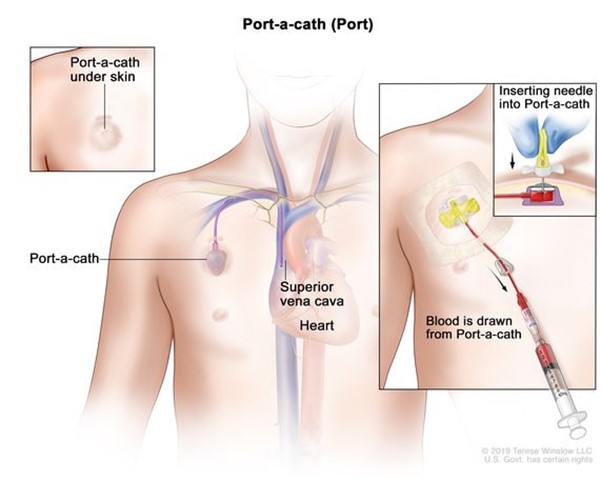
What is a portacath used for?
A port can be used to give you treatments such as chemotherapy, blood transfusions, or antibiotics. Ports can also be used when it is necessary to take samples of your blood for testing. This makes it possible for you to have your treatment without having to have needles frequently put into your veins. You can go home with the port in, and it can be left in place for weeks or months or, for some people, years. A port is more discreet than other types of central line because it lies completely under the skin and has no external parts.
How is the portacath put in?
You will have your portacath inserted in the operating theatre. This is usually done under local anaesthetic and sedation and takes about 45 minutes. You should feel relaxed and sleepy throughout the procedure, but you may feel some stinging when the local anaesthetic goes in and some pushing and pulling during the procedure. There may some brief periods of discomfort.
You will have an ultrasound and X-ray whilst you are having the procedure.
All the stitches are underneath the skin and dissolve on their own. You will have some glue over the wounds that acts as a dressing and will flake off after a week or two. The glue is water resistant but not fully waterproof.
Will it be sore?
You may feel a bit sore and bruised for a few days after the port is put in, a mild painkiller such as paracetamol will help with this. There may be some swelling and bruising around the port and this may take a few weeks to completely settle down.
How is the portacath used?
The port can be used immediately after it has been put in. When you are about to have treatment or have a blood sample taken, the skin over the port will be cleaned and a special needle, known as a Huber needle or gripper needle, is used to push through the skin and into the port - you may feel a slight sting as this is done. Your treatment will then be given down this needle. At the end of each treatment, the needle will be removed.
Care of your portacath
After each treatment a small amount of fluid is ‘flushed’ into the catheter so that it does not become blocked. The port will need to be flushed every 4 weeks if it is not being used. This is usually done by a nurse at the hospital or at your home. Apart from this, your port should not need any routine care at all.
Only Huber needles can be used with the portacath, do not let anyone use any other type of needle on your port.
The superglue dressing over the wounds is water resistant but not waterproof. For the first week or two after insertion try to avoid getting the wounds too wet (showers are fine but not baths). Once the wounds have healed it is safe to bath and to exercise as normal.
How is the portacath removed?
When you no longer need the portacath it will be taken out. This will be done in theatre using local anaesthetic and sedation is not normally required. The operation will take about 20 minutes. I will make a small incision through the old scar just above the port. Once the port and line are freed up then I will be able to remove them. I will close the wound with dissolvable stitches and put a superglue dressing over the wound.
A&E JOHNSTON LTD | Company number: 12101124 | Registered address: 7 Lindum Terrace, Lincoln, Lincolnshire, England, LN2 5RP
Cambridge Vascular Access: info@cambridgevascularaccess.com
Copyright © 2022. All Rights Reserved.